Metal analysis of urine shows promise as a potential diagnostic tool for pancreatic cancer
Research from Barts Cancer Institute (Queen Mary University of London), the University of Oxford and Columbia University has revealed that the signature of metal ions present in urine samples is an accurate indicator of pancreatic ductal adenocarcinoma (PDAC), one of the deadliest types of cancer.
Detecting biochemical changes in urine
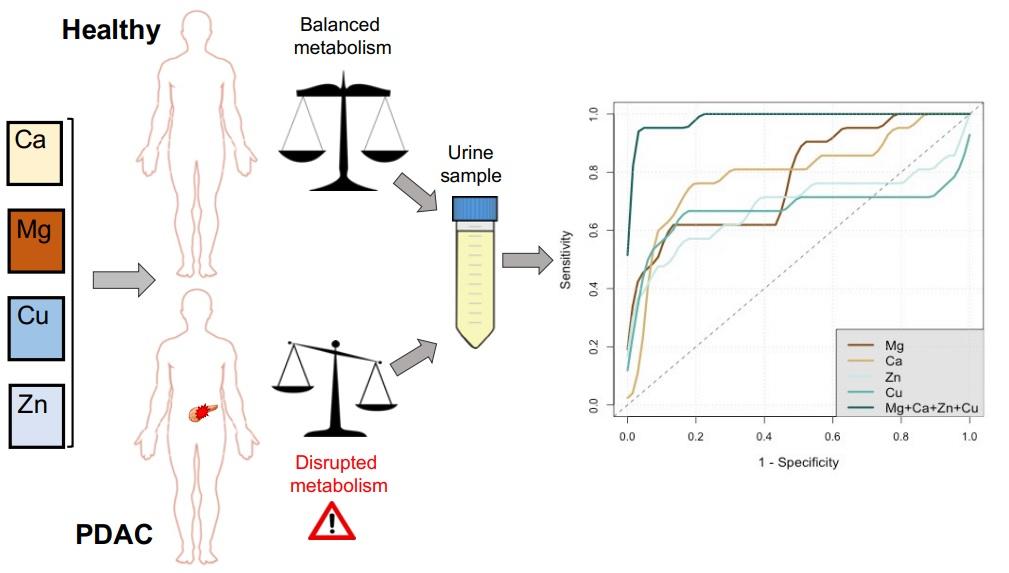
The study, funded by Pancreatic Cancer Action and published in Metallomics, took as its starting point the fact that cancer development leads to changes in biochemical reactions within the body. These imbalances, if measurable, can be powerful tools for cancer detection. The research team discovered that PDAC patients had significantly lower levels of urinary calcium and magnesium and increased levels of copper and zinc, when compared to healthy controls. A combined analysis of these essential metals was shown to be an accurate indicator of biochemical changes related to PDAC. The team also identified that the urine of PDAC patients has higher levels of a particular isotope of zinc (‘light zinc’) compared to healthy controls.
Senior author on the study Professor Tatjana Crnogorac-Jurcevic, from Barts Cancer Institute, said:
“We are very excited about our findings, and hope that we will be able to continue this work and further validate obtained results.”
Non-invasive detection
The discovery could signal the possibility of a new and completely non-invasive test for pancreatic cancer, of which PDAC is the commonest form, responsible for over 90% of pancreatic cancers.1 Although it accounts for only 3% of new cancer cases, pancreatic cancer accounts for 6% of cancer deaths in the UK because it has an extremely poor prognosis; sadly approximately 9,200 people lose their lives to pancreatic cancer in the UK annually.2 No tests for early detection are currently available and as symptoms are usually non-specific, PDAC is normally diagnosed at a late stage when it is already locally advanced or has spread to other parts of the body. Any improvement in tests for early detection would therefore represent a breakthrough.
Lead author Dr Kathrin Schilling, from the Department of Earth Sciences, University of Oxford, said:
“Our results demonstrate for the first time a remarkable difference in essential metal and zinc isotope composition in urine between PDAC patients and healthy people.”
The findings indicate that urine metallomics – the analysis of the types of metal present in the body – is a promising approach for the discovery of biomarkers for detection of patients with PDAC non-invasively, using urine samples.
“As urine samples can be taken time and time again in a non-invasive way, we can start to talk about an effective method to screen and monitor high-risk groups for pancreatic cancer,” Dr Schilling added.
What are the next steps?
The next step will be to study the levels of metal elements in a larger number of urine samples as well as in pre-diagnostic urine samples, to see if changes in their levels can be detected before the symptoms of cancer appear. If the results are still promising, the metal biomarkers will then be tested in prospectively collected samples, in a real clinical scenario. Professor Crnogorac-Jurcevic is already leading the UroPanc clinical study, a £1.6m study of protein biomarkers in the urine of PDAC patients, funded by the Pancreatic Cancer Research Fund, and samples from this study will be ideal for further validation of the metal biomarkers.
This research was performed in collaboration with the Department of Earth Sciences at The University of Oxford, Professor Alex Halliday’s research group at the Lamont-Doherty Earth Observatory, Columbia University, New York, Queen Mary University of London’s Wolfson Institute of Preventive Medicine, and the Department of Paediatrics and Paediatric Infectious Diseases, Sechenov First Moscow State Medical University, Moscow.
1Pancreatic Cancer UK, https://www.pancreaticcancer.org.uk/information-and-support/facts-about-pancreatic-cancer/types-of-pancreatic-cancer/, Accessed April 2020.
2Cancer Research UK, https://www.cancerresearchuk.org/health-professional/cancer-statistics/statistics-by-cancer-type/pancreatic-cancer, Accessed April 2020.
Article adapted from original release from the University of Oxford.
Category: General News, Publications

David clayton 08/03/2022
I’m very worried after weight loss and being type 2 diabetic that I may have pancreatic cancer I’m waiting for blood results and have a ct scan how can I test my urine for problems?
Barts Cancer Institute 08/04/2022
We are very sorry to hear this. Professor Tatjana Crnogorac-Jurcevic is leading the UroPanc clinical trial (https://www.pcrf.org.uk/uropanc-study/) to test the accuracy of detecting protein biomarkers in urine samples of patients with pancreatic cancer. The clinical study is still ongoing (unfortunately the recruitment was hampered due to Covid), and the standardised urine test is under development. So at the moment, urine testing for pancreatic cancer is not available in clinical practice.