The impact of chemotherapy on immune cells in the tumour microenvironment
Research from Barts Cancer Institute (BCI), Queen Mary University of London, has revealed novel insights into the effects of chemotherapy on the tumour microenvironment (TME). The study, published today in Cancer Immunology Research, a journal of the American Association for Cancer Research, found that chemotherapy enhances the anti-tumour actions of immune cells within the TME and their ability to support immune responses against cancer.
Cancers are not just a mass of cancerous cells, but are rogue organs made up of many different cell types, including cells that form connective tissue and blood vessels, and immune cells. These non-cancerous cells have been recruited and corrupted by the cancer to help it grow and spread, and constitute what is known as the TME.
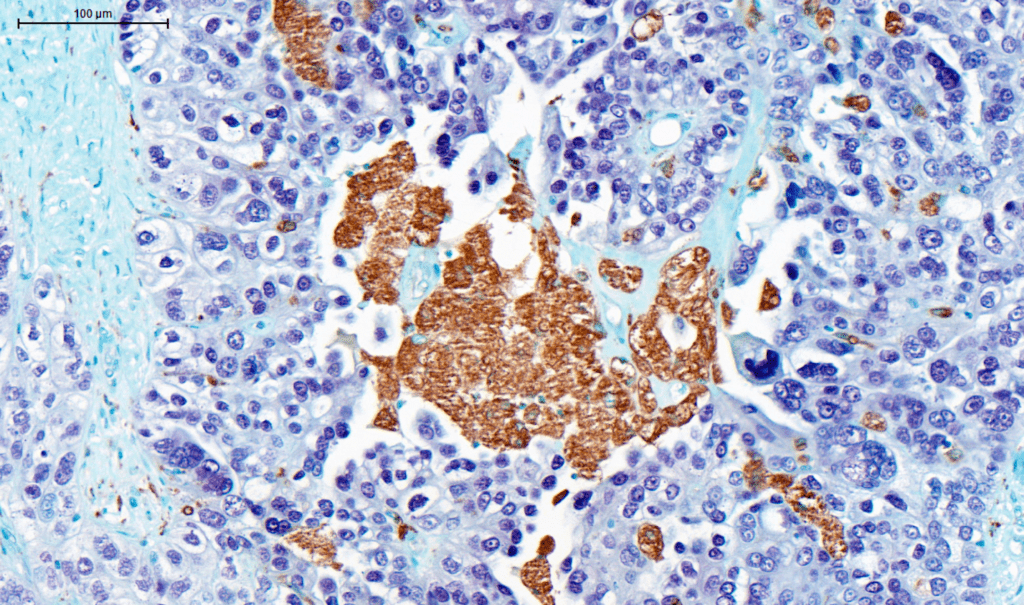
When treating cancer cells with chemotherapy, the cells within the TME are also impacted and previous research has shown that chemotherapy may activate immune cells within the TME to fight against the cancer. In this study, the team, led by BCI’s Professor Fran Balkwill, investigated the effects of chemotherapy on immune cells called macrophages, which are associated with poor survival across a variety of cancer types. The study focused on high-grade serous ovarian cancer (HGSOC) – the most common type of ovarian cancer.
Chemotherapy switches immune cells to anti-tumour mode
By comparing biopsy samples taken from the omentum (most common site of cancer spread in HGSOC) of 26 patients prior to and after chemotherapy, the team found a significant reduction in the number of macrophages present in the tissues following treatment. Further investigations in samples from other HGSOC patients revealed that chemotherapy switched the remaining macrophages from a pro-tumour to an anti-tumour mode, which may stimulate the patient’s immune response against the cancer.
The effects of chemotherapy on macrophages observed in patient samples were also seen in preclinical mouse models of HGSOC previously developed by the team, which recapitulate many aspects of the human omental TME.
As macrophages are associated with poor survival in cancer, the team took their research a step further to determine whether eliminating all macrophages from the TME after chemotherapy could prolong disease-free survival in the preclinical mouse models. To their surprise, removing all macrophages shortly after the completion of chemotherapy caused the mice to relapse quicker. Following three doses of chemotherapy, the macrophages had switched to an anti-tumour mode, and so eliminating the macrophages from the TME actually inhibited the immune response against the tumour and resulted in poorer survival outcomes.
The research was funded by Cancer Research UK, the Wellcome Trust and Wellbeing of Women.
Implications for ovarian cancer treatment
Chemotherapy and surgery are currently the main treatment options for patients with ovarian cancer. Despite chemotherapy working well initially, many patients experience relapse due to the development of resistance against these drugs.
Professor Balkwill said:
“This study enhances our understanding of the impact of chemotherapy on macrophages and other aspects of the immune response. As our work was driven by results first obtained in patient samples and we were able to replicate the findings in our mouse models, we could investigate hypotheses and obtain data that have translational significance.”
“We now have effective preclinical models of treatment and relapse that can be used to help identify treatments that build upon the tentative immune response triggered by chemotherapy.”
Ultimately, the team hope that their models could help to identify new drug combinations that harness the initial immune-boosting effects of chemotherapy to reduce the number of required chemotherapy doses, minimise toxic side effects and improve survival for patients with ovarian cancer.
The results of this study along with previous findings from the team are being presented today during the poster session of the AACR Annual Meeting 2021.
Category: General News, Publications

No comments yet