New study suggests promising approach for treating pancreatic cancer
Scientists at Queen Mary's Barts Cancer Institute have identified cells that drive the spread of pancreatic cancer and have discovered a weakness in these cells that could be targeted using existing cancer drugs. The findings, published in Science Advances and funded by Barts Charity and Cancer Research UK, suggest a new therapeutic strategy that could hold promise for this stubbornly hard-to-treat disease.
Pancreatic cancer is an extremely hard-to-treat type of cancer with an average five-year survival of just 7%. More than half of people are diagnosed after the disease has already spread to other parts of the body – a process called metastasis that ultimately leads to most cancer deaths. It's crucial that we find ways to treat this stage of the disease and to stop the spread in the first place if we are to improve the poor outlook for people with pancreatic cancer.
“Pancreatic cancer remains one of the deadliest cancers and current treatments are not working well. To improve these, we urgently need to understand the disease better,” comments Professor Victoria Sanz-Moreno, group leader at Barts Cancer Institute and senior author of the new study.
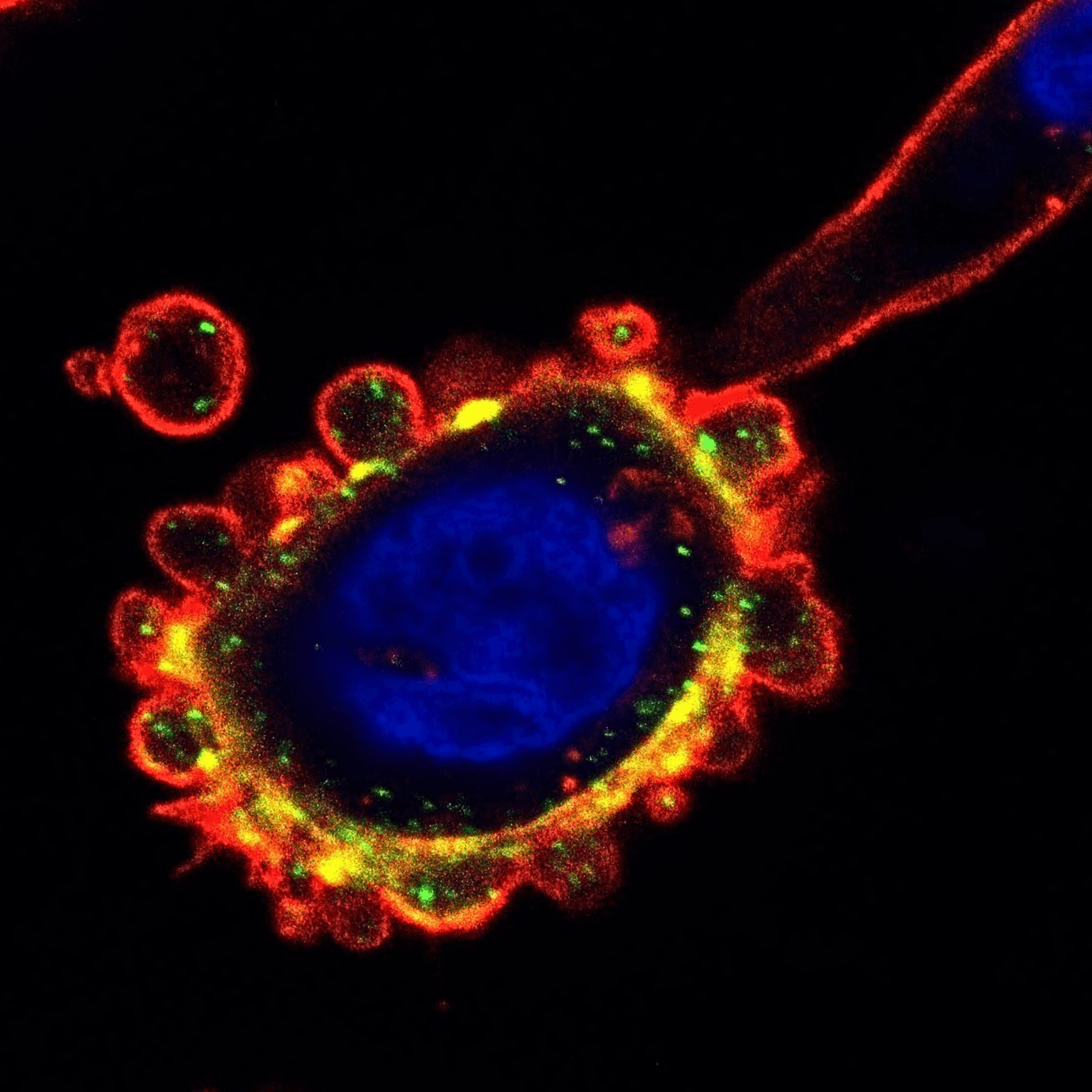
“Amoeboid cancer cells are always bad news”
To reach distant organs, cancer cells must propel themselves through the body. Professor Sanz-Moreno previously discovered that some migrating tumour cells adopt a style of movement called amoeboid migration.
“In other cancers we’ve looked at, amoeboid cells are always bad news,” Professor Sanz-Moreno explains. “They are linked to a poor outlook in the patients where we find them because they are aggressive, invasive, and they generate an immune response around them that helps rather than kills tumours.”
Until now, whether amoeboid cells existed in pancreatic cancer has been unclear. But in the new study, Professor Sanz-Moreno and her team revealed that they play an important part in pancreatic cancer’s ability to spread and suppress the immune system. What’s more, they identified an important weakness in these cells that could enable us to target them using existing cancer drugs.
“Pancreatic cancer remains one of the deadliest cancers and current treatments are not working well ... we urgently need to understand the disease better.”
— Professor Victoria Sanz-Moreno
A promising new target for pancreatic cancer treatment
The team found that amoeboid cells in pancreatic cancer produce high levels of a molecule called CD73. Researchers know that this molecule can help cancer cells suppress the immune system – as such, nearly 60 clinical trials studying drugs that block CD73 are already underway across many different cancer types. But Professor Sanz-Moreno’s team is the first to link this molecule to amoeboid cells and their ability to drive cancer spread.
Working with AstraZeneca, the team tested the effect of blocking CD73 in amoeboid cells in lab models. They found that it reduced the spread of cancer to the liver and decreased the number of immune cells that supported the tumour, suggesting that blocking CD73 could present a promising way to fight the progression of pancreatic cancer.

The team also studied samples from patients with pancreatic cancer. They found that amoeboid cancer cells that produce CD73 are linked to a poor outcome and are present in a large amount of patients in the later stages of the disease. Intriguingly, however, they also found that small numbers of these cells are already present in people with early-stage pancreatic cancer, raising possibilities for blocking the spread of cancer before it can truly start.
“There’s a strong argument for targeting these cells late in the disease when they are most abundant – but what if we were also able to target them early in the disease?” Professor Sanz-Moreno asks. “Could we avoid some of the most aggressive behaviours of pancreatic cancer from an early stage?”
Looking to the future
Further study is now needed to evaluate whether this approach could be effective in patients. With more than 10,000 people diagnosed with pancreatic cancer in the UK every year, improving its stubbornly low survival even marginally could save many years of human life. Ongoing clinical trials testing CD73-targeting therapies in pancreatic cancer could hold important clues as to whether these drugs could be successfully harnessed in a different way to tackle cancer spread.
Professor Sanz-Moreno and her team are now investigating whether a similar link between amoeboid cells and CD73 exists in other cancer types, which could reveal further opportunities to harness CD73-targeting drugs. In particular, the group is searching for these cells in breast cancer. As the most common type of cancer in the UK and the 2nd most common cause of cancer death in women, finding a new way to tackle breast cancer could have a huge impact.
Working together to tackle pancreatic cancer
This study was built on extensive collaboration between teams at the Barts Cancer Institute to combine expertise in discovery, translational and clinical research.
“The Barts Cancer Institute was the perfect place to conduct these studies as there is so much expertise in pancreatic cancer for us to benefit from,” Professor Sanz-Moreno explains. “We’d like to thank Professor Fran Balkwill for helping to instigate our connection with AstraZeneca and supporting our work on lab models of pancreatic cancer, and Professor Hemant Kocher for providing his clinical expertise and valuable patient samples. We are also very grateful to Professor Clare Wells at King’s College London, who played a key role in the initial stages of this study and to Dr Fernando Calvo who performed intra-vital imaging studies when his lab was a the Institute of Cancer Research in London (now at IBBTEC in Spain).”
“The Barts Cancer Institute was the perfect place to conduct these studies as there is so much expertise in pancreatic cancer for us to benefit from.”
— Professor Victoria Sanz-Moreno
Professor Claire Wells, a group leader at King’s College London, says: “We started this project because very little is known about how pancreatic cancer spreads, and we wanted to understand more about how cell morphology relates to spreading behaviour. The Wells laboratory is delighted to be a part of the important work that has emerged, pushing the boundaries of our understanding of pancreatic cancer spread and how we might prevent it.”
Victoria King, Director of Funding and Impact at Barts Charity says: “The ability of cancer cells to spread to other parts of the body is one of the greatest clinical challenges to treating cancer. Our investment in cancer research at Queen Mary has helped to attract world-leading researchers to East London who are making scientific breakthroughs that could transform the lives of people with cancer. We are excited to see the insights presented in this study, which suggest a promising new approach for halting the spread of pancreatic cancer.”
Dr Claire Bromley, Senior Research Information Manager at Cancer Research UK, says: "Thanks to research, over one million lives have been saved from cancer since the 1980s, but improvements haven’t been equal across all cancer types. Pancreatic cancer remains hard to treat and survival hasn’t improved in the past 50 years. Research like this is vital to innovate new ways to treat pancreatic cancer, which is the fifth most common cause of cancer in the UK. The team’s discoveries offer a promising new route for drugs of the future. However, more research is needed before these findings can move from the laboratory bench to the bedside."
This work was made possible thanks to funding from Barts Charity, Cancer Research UK, and the National Institute for Health and Care Research (NIHR) Biomedical Research Centre based at Guy’s and St Thomas’ NHS Foundation Trust and King’s College London. No NIHR BRC funds were used for animal studies. Please see the paper for a full list of funders for all authors.
Category: General News, Publications

Ian Hart 19/10/2023
Lovely study
Professor Adrian Newland 20/10/2023
An elegant study and good to see these innovative approaches. Unfortunately, too late for my wife.
Bhakti Mehta 21/10/2023
A promising find 🙂